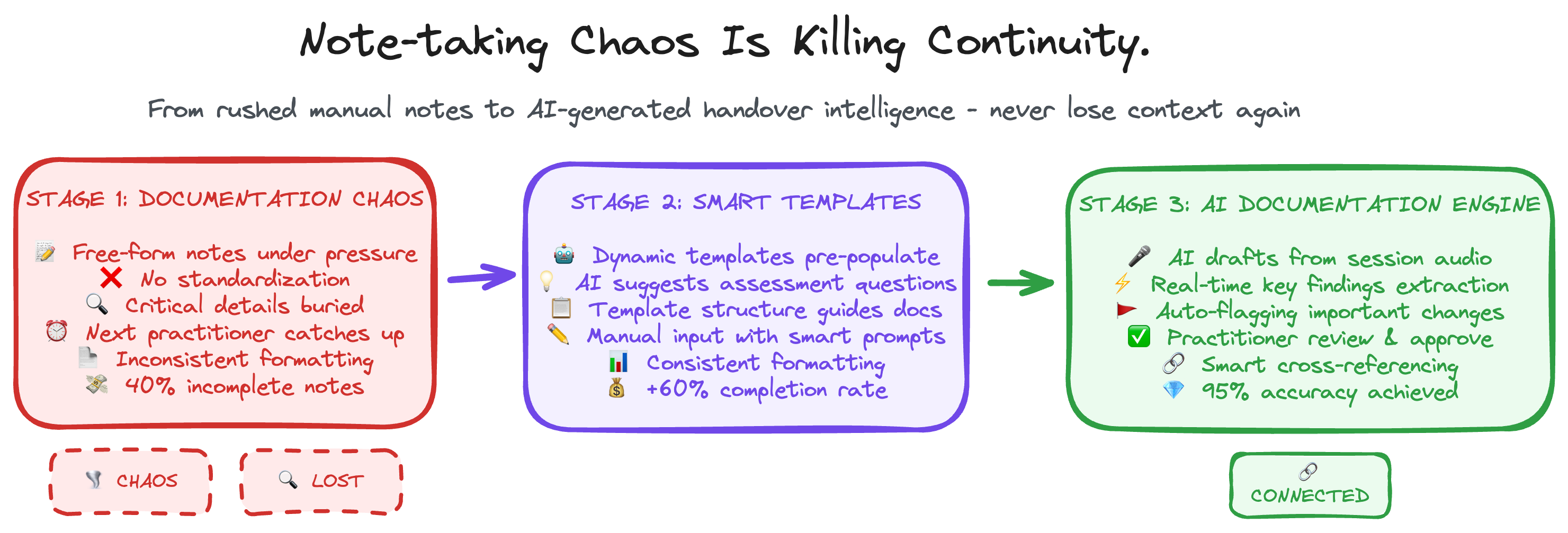
The Evolution Journey
From manual processes to intelligent automation, in three stages.
1
Manual Note Documentation
- Practitioners write notes during sessions disrupting flow
- Post-session documentation takes 15-30 minutes per patient
- Inconsistent note quality and detail across practitioners
- Risk of missing important patient information
- Time pressure leads to rushed or incomplete notes
2
Audio Recording with Manual Transcription
- Session recordings for later manual transcription
- Basic audio-to-text conversion requiring editing
- Template-based note structures for consistency
- Review and correction process for accuracy
- Integration with EMR systems for storage
3
AI-Powered Intelligent Documentation
- Real-time AI transcription with medical terminology recognition
- Automatic extraction of key clinical information
- Structured note generation following professional standards
- Integration with assessment tools and outcome measures
- Quality assurance with practitioner review and approval
Key Benefits
Significantly reduced administrative time per patient
More focused patient interactions without note-taking distractions
Consistent, comprehensive documentation quality
Better clinical decision-making through detailed records